Book Now
Services

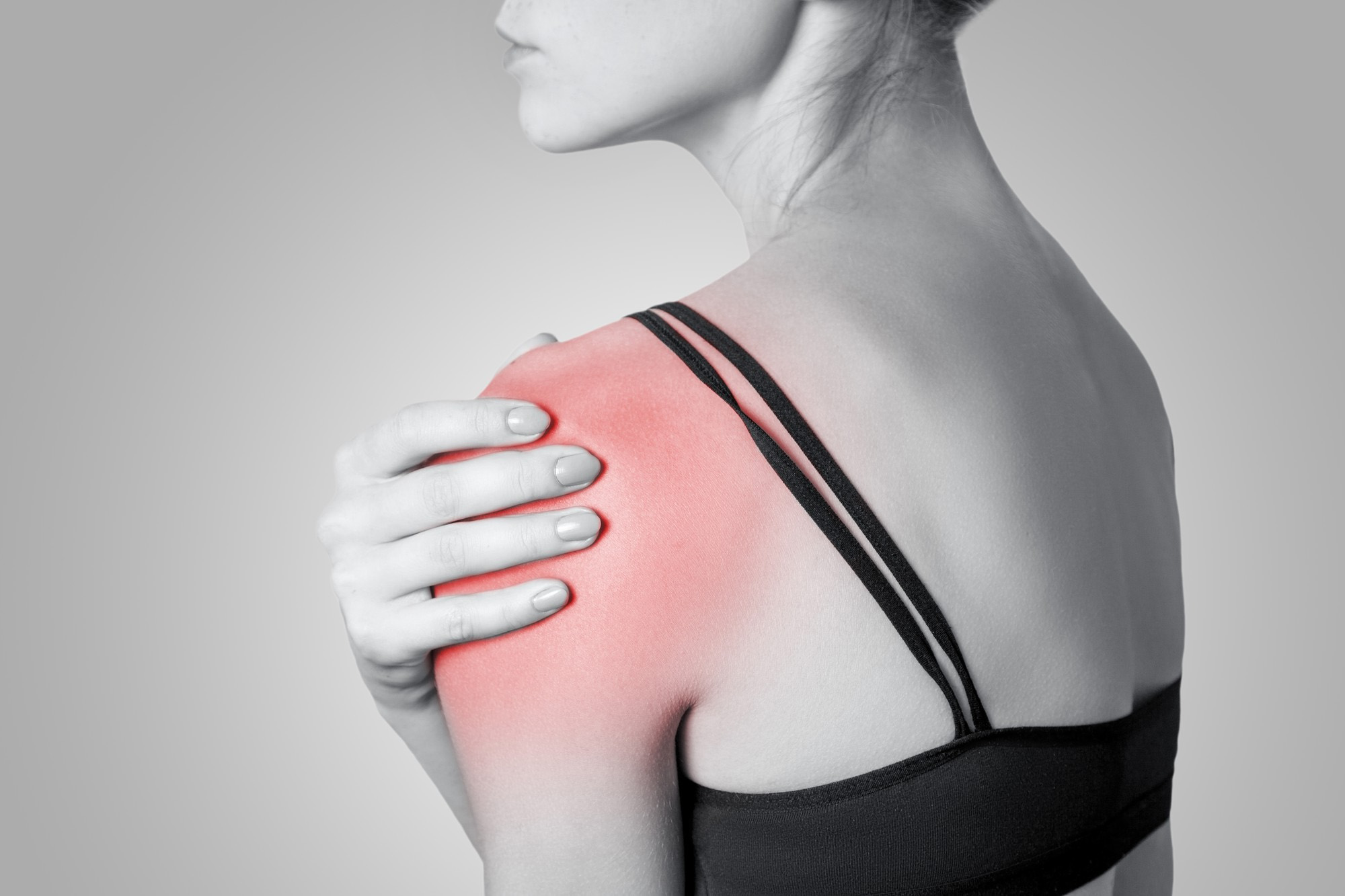
Frozen Shoulder
Frozen shoulder, also called adhesive capsulitis, happens when the shoulder capsule thickens and tightens, causing stiffness and pain in the shoulder.
Symptoms
The hallmark sign is not being able to move your shoulder – either on your own or with the help of someone else
Dull or aching pain, worsening with arm movement
Pain, usually in the shoulder area, and sometimes the upper arm
For some, the pain worsens at night and may disrupt sleep
Frozen shoulder typically develops slowly, and in three stages. Each may last for months. It then goes away slowly over the course of about a year.
Freezing stage
Any movement of your shoulder causes pain, slowly worsening, and your shoulder’s range of motion starts to become limited.
Lasts from 6 weeks to 9 months
Frozen stage
Pain may begin to diminish during this stage, but the stiffness remains or worsens making activities of daily living very difficult
Lasts 4 to 6 months
Thawing stage
The shoulder’s range of motion begins to improve.
Return to normal (or close to normal) motion and strength
Takes 6 months to 2 years
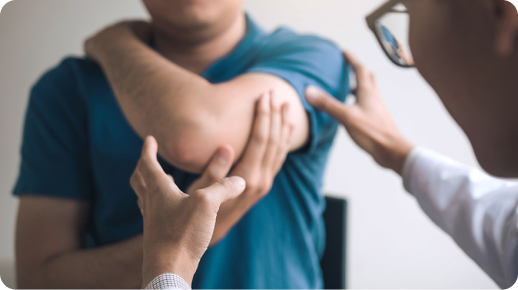
Causes
Frozen shoulder can develop when you stop using the joint normally because of pain, injury, or a health condition. Here are some risk factors:
Recovering from a medical condition or procedure that prevents you from moving your arm — such as a stroke or post-mastectomy
Most often in people with chronic diseases, such as diabetes, hypothyroidism, hyperthyroidism, Parkinson’s disease, and cardiac disease.
More common between the ages of 40 and 70
More often in women than in men
History of any shoulder problem, arm fracture, or other injury wherein full range of motion is not practiced
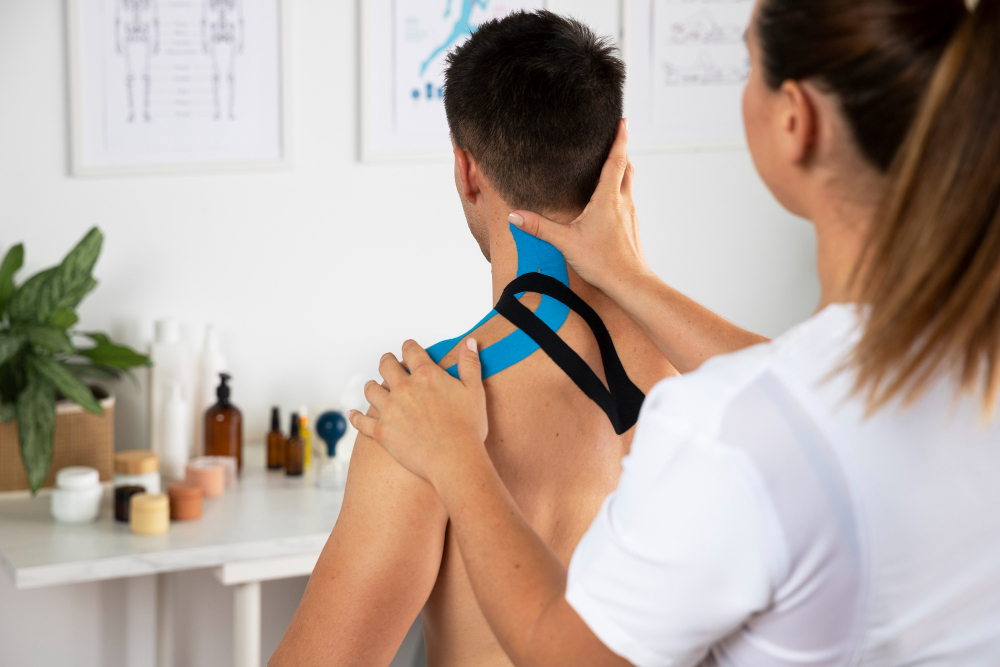
Treatment
Heat application to the affected area, to loosen the shoulder up, followed by gentle Physical therapy is a good option. Range of motion exercises will be taught by your therapist to help recover the shoulder’s mobility as much as possible.
Non-steroidal anti-inflammatory drugs to reduce pain and swelling.
Corticosteroid injections Cortisone is a powerful anti-inflammatory medicine that is injected directly into your shoulder joint to decrease pain and swelling, especially in the early stages of the condition.
Heat application should be done to optimize recovery.
Conservative treatment works 90% of the time; however, if these treatments are not working, surgery may be necessary to loosen the tight tissues around the shoulder.
Shoulder Manipulation under anesthesia- you are put under general anesthesia, and then your arm is moved into positions to loosen and stretch the tight tissue.
Shoulder Arthroscopy –using tubular, pencil-sized instruments inserted through small incisions around your shoulder, to cut through tight tissues and remove scar tissue and adhesions.
In many cases, manipulation and arthroscopy are both done to get maximum results. Most patients have very good outcomes with these procedures. Although unusual, frozen shoulder can recur in the same shoulder, especially if a contributing factor like Diabetes is still present. Some people also develop it in the opposite shoulder. After surgery, physical therapy is necessary to maintain the motion that was achieved with surgery, and your commitment to therapy and continuously doing the exercise are very important in returning to all your daily and leisure activities.
Prevention
Stretching and strengthening are going to be your best defence against frozen shoulder. Even if you don’t have a shoulder problem now, the following stretching and strengthening exercises could save you from a major headache in the future.

