Tendinitis

A tendon is a strong, fibrous cord that joins muscles to bones. Tendonitis is an inflammation or irritation of a tendon.
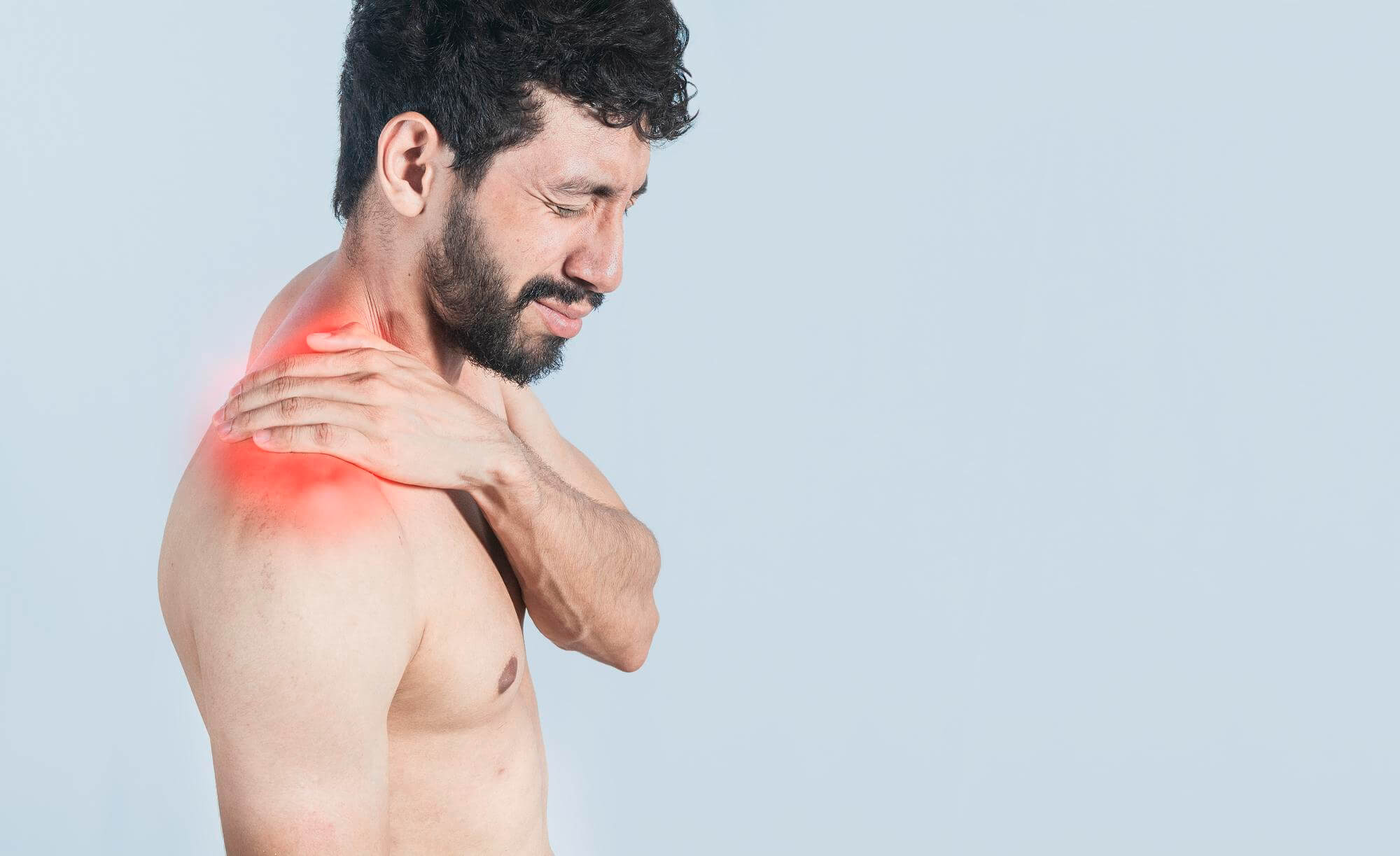
Tendonitis can make it difficult to move or use the affected joint by causing discomfort, soreness, and minor swelling around the area.
Any tendon in the body can develop this illness, but the shoulder, elbow, wrist, knee, and heel are among those that experience it most frequently.
Symptoms
Depending on the exact tendon involved and the level of inflammation, tendinitis symptoms can change.
However, some common symptoms associated with tendonitis are mentioned below.
- Pain: Tendonitis typically causes pain at or around the affected tendon, which may worsen with movement or when pressure is applied to the area.
- Tenderness: The area around the inflamed tendon may be tender to touch.
- Swelling: Mild swelling may occur in the area surrounding the affected tendon due to inflammation.
- Stiffness: Limited range of motion and stiffness in the affected joint may result from the inflammation of the tendon.
- Weakness: The affected joint or muscle may feel weak, making it difficult to perform certain activities or movements.
- Redness & Warmth: In some cases, the skin over the affected tendon may appear red and feel warm to the touch.
A medical history, physical examination, and, occasionally, imaging tests are used to diagnose tendinitis. Here are some steps a healthcare professional may take to diagnose tendonitis:
- Medical History: The healthcare provider will ask about the patient's symptoms, the activities that cause or worsen the pain, any previous injuries, and any history of similar issues. This information helps the healthcare provider determine if the patient's symptoms align with tendonitis or another condition.
- Physical Examination: The healthcare provider will examine the affected area, checking for tenderness, swelling, redness, and warmth. They may also ask the patient to perform specific movements or apply resistance to assess the pain and range of motion. These tests can help identify the affected tendon and rule out other potential issues, such as fractures or joint problems.
- Imaging Tests: Imaging studies could be required in some situations to confirm the diagnosis or rule out alternative illnesses. These tests may include:
- X-rays: While X-rays do not show tendons, they can help rule out bone abnormalities or arthritis that may be causing the pain.
- Ultrasound: An ultrasound can detect symptoms of inflammation, thickness, or rips and give a real-time image of the injured tendon.
- Magnetic resonance imaging (MRI): An MRI can provide a detailed view of the tendon and surrounding structures, helping to identify tendonitis or other issues, such as tendon tears or bone injuries.

Treatment for tendonitis typically focuses on reducing inflammation and pain, allowing the affected tendon to heal, and preventing future occurrences. Some common treatment approaches for tendonitis include:
- Rest: Avoiding activities that cause pain or exacerbate the condition is crucial for allowing the inflamed tendon to heal. It may be necessary to modify or temporarily discontinue the activity that led to tendonitis.
- Ice: Applying ice to the affected area for 15-20 minutes several times a day can help reduce inflammation and pain. Make sure to wrap the ice or ice pack in a towel to protect the skin.
- Compression: Wearing a compression bandage or brace can help provide support and reduce swelling around the affected tendon.
- Elevation: Elevating the affected area above the heart level can help minimize swelling and inflammation
- Anti-Inflammatory Medications: NSAIDs, which are sold without a prescription, can help lessen pain and inflammation.
- Physical Therapy: A physical therapist can recommend specific exercises to strengthen the muscles around the affected tendon and improve flexibility. This can help alleviate stress on the tendon and prevent future occurrences of tendonitis.
- Corticosteroid Injections: In some circumstances, a medical professional could advise corticosteroid injections to lessen pain and inflammation.
- Extracorporeal Shock Wave Therapy (ESWT): This non-invasive treatment uses high-energy shock waves to stimulate the healing process in the affected tendon. ESWT may be considered for cases of chronic tendonitis that have not responded to conservative treatments.
- Surgery: In rare cases, when conservative treatments have not provided relief or the tendon is severely damaged, surgery may be necessary to repair the tendon.
- Preventive Measures: Adopting preventive strategies, such as maintaining overall muscle strength and flexibility, using proper techniques during sports or work-related activities, and gradually increasing the intensity of physical activities, can help avoid overloading the tendons and reduce the risk of developing tendonitis.

Causes
Tendonitis is typically caused by factors that place excessive stress or strain on the tendons. Some common causes of tendonitis include:
- Overuse: Repetitive movements or activities can cause small, cumulative injuries to the tendons, leading to inflammation and irritation. This is particularly common in athletes or individuals who engage in regular physical activities that involve the same body parts.
- A Sudden Increase in Activity: Increasing the intensity or duration of physical activity too quickly without allowing the body to adapt can put undue stress on the tendons, resulting in tendonitis.
- Poor Technique or Biomechanics: Incorrect form or technique during sports, exercise, or work-related activities can place excessive strain on the tendons, increasing the risk of tendonitis.
- Muscle Imbalances: The tendons might be subjected to additional tension from weak or tight muscles, increasing their sensitivity to inflammation and damage.
- Age-Related Degeneration: Tendons become less elastic and more prone to damage and inflammation as people age.
- Posture: Poor posture can result in uneven distribution of force on the tendons, contributing to the development of tendonitis.
- Inadequate Warm-Up or Stretching: Tendon injuries, including tendonitis, can become more likely if you don't adequately warm up or stretch before indulging in physical activity.
- Underlying Medical Conditions: Tendonitis risk might be increased by certain medical disorders including rheumatoid arthritis or diabetes.
- Footwear & Equipment: Wearing inappropriate or ill-fitting footwear or using poorly designed or worn-out sports equipment can contribute to tendonitis by altering the mechanics of movement and placing excess stress on the tendons.

